
As much as you love how your glasses improve your vision, you wish you could go back to your glasses-free days. Perhaps you want to sport a new makeup look and your glasses get in the way of the overall effect. Or maybe you just want to see clearly without wearing your eyeglasses. Whatever the case, contact lenses present the perfect solution.
With these small, optic devices, you can try out that new makeup tutorial, wear your favorite pair of sunglasses, or participate in sports without worrying about the glasses breaking or falling off. But did you know that you can choose from a few different contact lens options?
Below, we’ll discuss both soft and hard contact lenses. Read on so you can discover which lens option will work best for your eyes.
Hard Contact Lenses
Commonly known as hard contact lenses, rigid gas permeable lenses (RGPs) are rigid lenses that are made from oxygen-permeable polymers. The first hard lenses were made of glass and were invented over 100 years ago. However, modern hard lenses were created in the 1970s.
Original hard lenses were difficult for people to wear since the lenses restricted oxygen flow to the eyes. Once RGPs were invented, hard lenses allowed more oxygen to flow into the wearer’s eyes, reducing dryness and making the lenses more comfortable to wear.
However, these lenses will feel a little uncomfortable when you first wear them. After time, your eyes will adapt and you’ll feel completely comfortable wearing RGP lenses.
Hard lenses replace the natural shape of your cornea, so they appear smaller in size than soft lenses. Because of their makeup and size, hard lenses can actually correct vision for those individuals who suffer from astigmatism. Depending on the severity of your astigmatism, hard lenses may be your only contact lens option.
RGPs also provide the following benefits:
- They are easy to clean, care for, and wear.
- They are incredibly durable, so you don’t have to worry about them tearing as easily as soft contacts.
- They don’t dehydrate, so your eyes won’t dry out as easily from wearing them.
- They come in several different colors.
- They hold their shape, so you are less likely to feel discomfort as you wear them.
- They come in both multifocal and bifocal forms to further enhance your vision.
Like all forms of corrective vision, RGPs do have their disadvantages. For example, their small size makes it easier for them to dislodge from your eyes. They can also get scratched, which can inhibit your vision. Additionally, debris can build up underneath the lenses and create discomfort or inhibit your ability to see clearly.
Soft Lenses
Thanks to modern technology, soft lenses have become some of the most commonly used contact lenses to correct people’s vision. These lenses are made of malleable plastic polymers, so they mold to your eye’s shape. Additionally, these lenses are larger than RGPs. In fact, they are large enough to cover both your cornea and your iris.
In the 1960s, Otto Wichterle, a Czech chemist, invented soft contact lenses. He used a hydrogel and a homemade device to form the lenses. The molding apparatus was actually made from a children’s building kit, a bell transformer, a bicycle dynamo, and molds and glass tubing that he created himself.
Over time, chemists and other eye doctors adjusted the monomers and polymers used in soft lenses to create the lenses we use today.
These lenses are most commonly made of silicone hydrogel to increase each lens’s oxygen permeability and comfort. Soft lenses also provide the following benefits to wearers:
- They are less likely to get dust and debris stuck under them if you clean and wear them properly.
- They feel comfortable almost immediately, unless you put them on inside out.
- They are perfect for irregular wear because they’re so easy to adapt to.
- They come in tinted versions so you can see them more easily.
- They hardly fall out of your eyes, so they’re ideal if you play sports.
- They require a shorter adjustment period
As with RGPs, soft lenses come with their disadvantages as well. For example, soft lenses are less sturdy than RGPs, and you can easily tear them if you aren’t careful. These lenses may also dry out, so your eyes could feel dry until you moisten them. Soft lenses also absorb chemicals (like chlorine from a pool) more easily, which could cause irritated eyes.
Hybrid Lenses
You can also ask your eye doctor about hybrid lenses. This lens option combines both RGPs and soft lenses to provide you with a more comfortable and accurate form of corrective vision. These lenses have a durable, RGP center with a soft skirt on the outside. The center also makes these contacts more breathable so your eyes take in more oxygen.
The RGP center enhances your vision and still corrects for astigmatism, while the soft outer skirt enhances how comfortable the lenses feel in your eyes.
Correct Your Vision in the Way That Serves You Best
Ready to correct your vision without bulky glasses? Get in touch with the All About Eyes location nearest you and schedule an eye exam. Tell the staff at the office that you’d also like to get a contact exam. Your eye doctor must perform a more in-depth eye exam to ensure you receive the right prescription for your contact lenses.
Additionally, this exam will allow your doctor to better determine which lens type best fits your specific eye shape. Schedule your appointment today and start the journey to clearer vision.

During the spring and summer seasons, you expect that your eyes will water a little as pollen levels increase. And if you live or work in an environment that has allergens in the air, you’re no stranger to having slightly pink or red eyes. In fact, this coloration might be normal for you if you suffer from allergies.
But if that unsightly pink or red color doesn’t go away, you may wonder if something else has caused this effect. If the coloring is accompanied by itching and a few other symptoms, you may even start to worry that you’ve developed a serious eye issue. More than likely, however, you’ve contracted a case of conjunctivitis—commonly known as pink eye.
Below, we’ll discuss pink eye in depth. We’ll let you know what this condition is, what its causes and symptoms are, and if it poses any long-term risks to your ocular health.
The Basics
Pink eye is a common condition in both children and adults. It can spread fairly quickly and can make your eyes feel incredibly irritated. Simply put, pink eye is an infection or inflammation in your eye’s conjunctiva. This thin, transparent membrane covers the white portion of your eyeball and the inside of your eyelids. Small blood vessels rest in the conjunctiva as well.
This membrane is important to proper eye function. The conjunctiva produces tears and mucus to lubricate your eyes, keeping them moist and allowing you to see properly. The conjunctiva also protects your eye from microbe- and foreign-object-induced damage.
When this membrane becomes exposed to bacteria, dirt, debris, and other irritants, the tears and mucus typically wash the debris away. However, the membrane can become so irritated that the blood vessels inflame and turn your eyes pink or red.
The Causes
Typically, a viral or bacterial infection causes pink eye. If you develop this version of pink eye, you’ll need to seek medical attention for treatment. If you have a viral form of conjunctivitis, you can easily spread it to another person.
Aside from a viral infection, several other factors can cause conjunctivitis. Other causes of pink eye include:
- Chemical exposure
- Allergies
- Fungi
- Parasites
- STIs
- Foreign objects
Certain diseases can also cause conjunctivitis. Additionally, newborn babies are at high risk for contracting conjunctivitis because they are exposed to bacteria as they pass through the birth canal. However, doctors must treat newborns immediately, otherwise the pink eye can severely damage the child’s eyesight.
The Symptoms
As previously mentioned, conjunctivitis causes your eyes to turn a bright pink or red color. However, the discoloration alone doesn’t usually indicate that you have conjunctivitis. If you do have the condition, you’ll manifest a few other symptoms, including:
- Itchy eyes
- Teary eyes
- Gritty feeling in your eyes
- Burning eyes
- Swelling
- Blurry vision
You may also experience an increased sensitivity to light if you have pink eye. Additionally, you may notice a green, white, or yellow discharge in the corners of your eyes. The green or white discharge will usually stay in the corners of your eyes and lead to excessive tearing.
However, the yellow discharge is thicker and will crust over your eyelashes. This symptom usually manifests in the evenings or early mornings during or after sleep.
The Treatment
If left untreated, viral pink eye can lead to more serious health risks. For example, the condition can cause your cornea to become inflamed, which in turn can affect your vision. If your cornea becomes scarred, you could suffer from more serious vision loss.
Fortunately, your optometrist can treat the condition fairly easily. Allergy-induced pink eye simply requires you to reduce your exposure to allergens. If you are unable to eliminate allergens (such as those found in outside air), an allergy pill such as Zyrtec could clear up your symptoms.
For bacterial conjunctivitis, your optometrist will likely prescribe antibiotics to eliminate your symptoms. Sometimes, your eye doctor may give you eye drops that contain a steroid to further lower your discomfort and help your eye heal.
Preventative Measures
To avoid developing conjunctivitis or contracting the condition again, take the following preventative steps:
- Wash your hands with warm, soapy water before you touch your eyes.
- Wash your bedding frequently and in hot water. You should also wash all towels and other linens immediately after an infection has cleared up.
- Wear contact lenses for the proper amount of time. Wearing contacts longer than the recommended time frame significantly increases your risk for developing pink eye.
- Never share makeup with another person.
If you manifest any of the symptoms of pink eye, see an eye doctor as soon as possible. He or she can prescribe you the appropriate antibiotic eye drops to clear the infection. Additionally, your eye doctor can provide you with additional tips to avoid contracting conjunctivitis again in the future.
To maintain good eye health throughout your life, you’ll also want to schedule regular eye appointments with your optometrist. During these visits, your eye doctor can see what eye conditions you are at risk for and provide you with effective treatment.
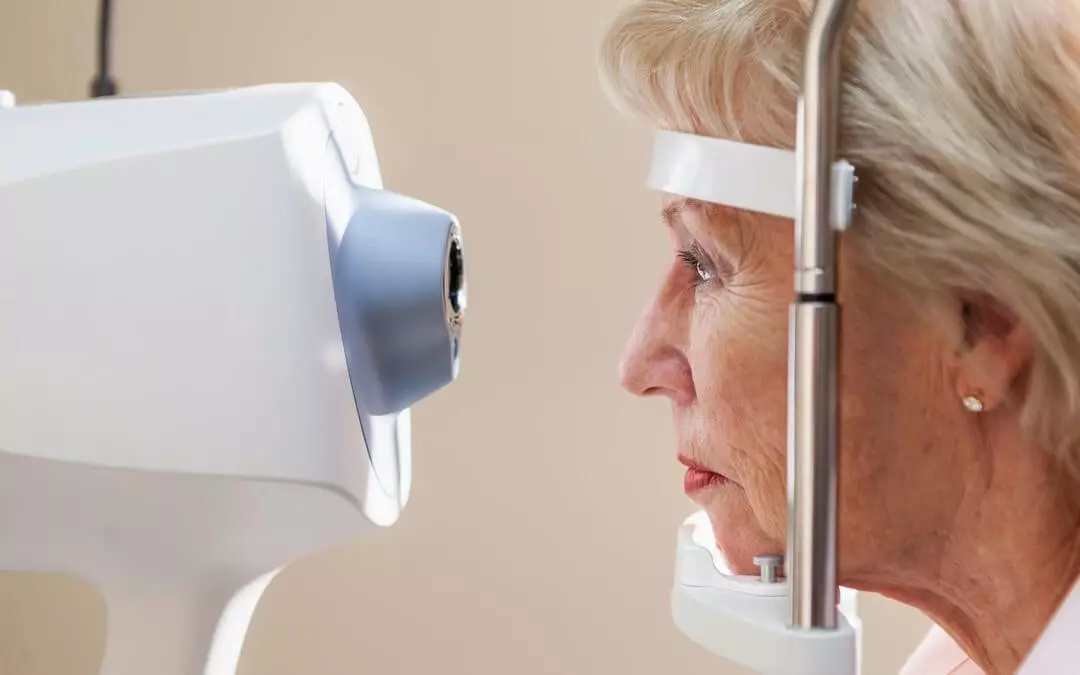
As you’ve aged, you’ve noticed that your eyes feel sore and tired more easily than normal. Maybe you’ve felt some slight pressure behind your eyes that doesn’t go away. Or perhaps your vision has started to blur gradually. Whatever the case, you know you should have your eyes checked to prevent more serious issues.
When you visit your eye doctor, he or she usually examines your eyes and tells you about your overall eye health. But during a visit, he or she may have mentioned that you are at risk for developing glaucoma.
You’ve heard about this eye condition, but you still don’t know as much about it as you’d like. Below, we’ll walk you through glaucoma: what it is, what its symptoms are, and how an eye doctor can help you cope should you ever develop it.
What Is Glaucoma?
Simply put, glaucoma refers to a condition in your eye that can cause damage to your optic nerve. The optic nerve transmits images from your retina to your brain so you can see properly. Glaucoma develops as a result of fluid and pressure buildup behind your eye.
The resulting damage interferes with your ability to see correctly. In fact, the American Academy of Ophthalmology states that not only is this condition the second leading cause of blindness in the US, but it is also the leading cause of blindness in individuals 60 years old and above.
The condition develops rather slowly, so even if you have glaucoma, you may not notice any of the symptoms immediately. However, the sooner you begin treating the condition, the lower your chances are of becoming blind later on.
Additionally, there are several different kinds of glaucoma you could develop. These types include:
- Open-angle glaucoma
- Congenital glaucoma
- Glaucoma suspect
- Secondary glaucoma
- Closed-angle glaucoma
- Normal-tension glaucoma
Open-angle glaucoma is the most common form found in adults. And unfortunately, it is one of the more difficult forms to treat—especially because most people who have this condition don’t have high eye pressure when they have their eyes examined initially.
What Are the Symptoms of Glaucoma?
Regardless of which form of glaucoma you are at risk for, the condition still manifests similar symptoms. As you care for your eyes, take note of any of the following symptoms:
- Suddenly blurry vision
- Blank spots on your peripheral vision
- Pressure behind the front part of your eye
- Headaches
- Nausea
- Vomiting
- Severe eye pain
- Halos around lights
- Tunnel vision
- Red eyes
Additionally, individuals with glaucoma may have hazy eyes. This symptom is particularly prominent in children, but adults can still manifest it. If you’ve noticed any of the above symptoms, make an appointment with your eye doctor as soon as possible.
How Can an Ophthalmologist Diagnose This Condition?
Once you meet with your ophthalmologist, he or she will perform a few different tests and use various tools to diagnose the condition.
Pachymeter
This tool measures your central corneal thickness (CCT). Your eye doctor will anesthetize your eyes before the procedure begins. Then, he or she will place a probe perpendicular to your cornea. The probe will then measure your CCT and evaluate your intraocular pressure (IOP) levels. If you have a thin CCT and high IOP levels, you are more at risk for developing—or may already have—glaucoma.
Tonometer
The tonometer is a tool that also measures your eye’s pressure. Your eye doctor will also use a numbing agent (usually a drop) to anesthetize your eye. Your head and chin rest on a support while a slit-lamp shines in your eye. This lamp allows your ophthalmologist to see a magnified view of your eye. You’ve likely had this tool used on you if you’ve had an eye exam before.
He or she may even perform a gonioscopy, opthalmoscopy, or visual field test to further examine your vision and determine the severity of your glaucoma.
Your eye doctor may even use new imaging technology to examine and evaluate your optic nerve. These images let your eye doctor review your eye over a period of time to determine how quickly or slowly your class of glaucoma is progressing.
What Kinds of Treatment Are Available?
Unfortunately, there is no cure for glaucoma. However, there are several kinds of effective treatments available. The kind of treatment your eye doctor prescribes depends entirely on which type of glaucoma you have and how severe it is.
Typically, your eye doctor will prescribe glaucoma medication (usually in the form of medicated eye drops). The medication lowers your IOP either by reducing the fluid buildup in your eye or by helping the fluid flow out of your drainage angle better. Your ophthalmologist may even recommend the following surgeries to treat your glaucoma:
- Laser iridotomy
- Laser trabeculoplasty
- Peripheral iridectomy
- Aqueous shunt surgery
- Trabeculectomy
Your eye doctor will only recommend these treatment options if medicated drops won’t reduce the symptoms.
If you’ve manifested any of the symptoms listed above, get in touch with your ophthalmologist as soon as possible. He or she can perform some of the exams discussed above to determine if you do have glaucoma. Additionally, he or she can provide you with effective treatment to help you manage the condition so you can see better and live a life with little or no symptoms.
Remember, to keep your eyes healthy and to prevent serious eye issues from developing too far, you should see your eye doctor regularly. Schedule a routine eye exam with you eye doctor so he or she can diagnose any eye issues and treat these problems in a timely manner. Your ophthalmologist can also provide you with additional tips you need to maintain good eye health over your lifetime.

Pause for a moment and think about your vision. Are you someone who’s worn glasses or contacts most of your life? Have you been lucky enough not to need vision aids? Because you’ve used your eyes every day of your life, you know your sense of sight better than anyone else. Your familiarity with your own eyes makes you the best person to notice small changes in your vision.
Now take a quick moment to consider the following questions. Do you have tiny black spots or lines in your eyes? Do those shapes follow your eyes as you look around but resist being focused on directly? Do those dots or squiggles become especially prominent when you look at a blank, bright surface, like a white sheet of paper or the clear, blue sky?
If those symptoms sound familiar, you have likely developed floaters. Read on to learn about what these small changes in your vision mean for your eyesight.
Why Do Floaters Occur?
In most people, floaters are a natural part of the aging process. They develop when the liquid in your eye, known as vitreous, shrinks and changes consistency over time. The cells in vitreous fluid clump together as it shrinks, and those clumps create tiny shadows that look like they’re sitting at the front of your eye. In reality, these clumps float around inside your eye, which explains why they move around.
Eventually, most age-related floaters, like those described above, will sink to the bottom of your eye and out of your field of vision. These floaters occur in almost everyone, but if you have diabetes or nearsightedness or you underwent a cataract operation, you may have a higher occurrence of floaters.
Age-related floaters usually only show up a few at a time, and they typically aren’t accompanied by other symptoms. They seem annoying, especially at first, but they are benign and shouldn’t cause you to worry.
What Symptoms Could Mean Floaters Are More Serious?
Less commonly, floaters indicate more serious vision issues. Other symptoms usually accompany these floaters, such as:
- A large number of floaters appearing in a short time
- A loss of peripheral vision
- Unexplained flashes of light, especially in your peripheral vision
These symptoms could be early signs of significant changes within the eye, so you should make an appointment with an eye doctor as soon as possible if you notice these symptoms.
At your appointment, make sure to mention these symptoms and provide an approximate timeline for when they started. An optometrist can take a closer look at your eyes, determine what problems affect your vision, and recommend treatment.
Your eye doctor looks to see if your floaters have developed due to one of the following conditions.
Posterior Vitreous Detachment
Vitreous fluid rests in the back of your eyes. It occupies the large open space behind the cornea and lens. As noted above, vitreous fluid shrinks over time. In some people, as this shrinkage occurs, the vitreous fluid makes less contact with the retina, a vision center on the back of the eye. This decrease in contact is called posterior vitreous detachment.
According to a study published in the medical journal Ophthalmology, posterior vitreous detachment is the reason for a sudden appearance of floaters or flashes of light in about 40 percent of patients who report those symptoms. An eye doctor diagnoses posterior vitreous detachment by performing a dilated eye exam.
Most cases of posterior vitreous detachment are not serious and do not cause long-term sight problems.
Retinal Tears
Sometimes when the vitreous fluid pulls away from the retina, the force strains the retina and creates tears or holes. According to the same study cited above, retinal tears occur in about nine percent of patients.
Retinal tears are more serious and can have long-term effects on eyesight. They are one reason you should have your vision checked immediately if you notice the symptoms in the bulleted list above.
Ophthalmologists may use lasers or a special freezing treatment to seal holes in torn retinas. These treatments cause minimal discomfort and can be done in the eye doctor’s office.
Retinal Detachment
Retinal tears often lead to a more serious eye problem called retinal detachment. This problem develops when vitreous fluid passes through the retinal tear. The fluid builds up behind the retina and separates it from the underlying tissue. A detached retina cannot properly focus light, so vision becomes blurry, and blindness can eventually occur.
In patients with retinal detachment, eye surgery is necessary to preserve vision. Many surgeries for retinal detachment take place in an operating room, but some can be performed at an ophthalmologist’s office. The American Academy of Ophthalmology reports that these surgeries have an 80 to 90 percent success rate.
Should You Worry About Floaters?
Although floaters can be bothersome, in most people they aren’t cause for concern. You can make sure the floaters in your eyes are not problematic by watching for the extra symptoms listed above and by making regular visits to an eye professional.
Remember to take care of your sight between eye appointments too. Wear your glasses or contacts as directed, and protect your eyes with sunglasses. Watch for sudden changes in your vision, and consult with an eye care professional if you notice any.

As you sit at your desk and work on your computer, you notice that your eyes sting, feel tired, or ache. You may have noticed these sensations for a few days, and they don’t seem to improve over time. You’d like to reduce the pain you feel, but you aren’t sure what has caused your discomfort.
More than likely, you’ve strained your eyes. Though eyestrain is fairly common among most adults (and even though it doesn’t damage the eye), it is still a nuisance to deal with. Below, we’ll discuss everything you need to know about eyestrain so you don’t have to suffer from this ailment longer than necessary. Read on to learn what causes the condition, what its symptoms are, and how to treat and prevent it.
What Is Eyestrain?
Essentially, eyestrain is a term that describes most discomfort, pain, and fatigue you feel in your eyes after you’ve used them for an extended period of time. You can strain your eyes doing a number of different tasks and activities for a long time, such as:
- Driving (especially in the dark)
- Writing
- Reading
You can also strain your eyes if you expose yourself to bright lights, such as those emitted from smartphones, computer and tablet screens, and television screens. The longer you stare at a screen or the longer you go without moving your eyes around, the higher your risk is for developing eyestrain.
Additionally, if you work on a computer or other electronic device, you are more likely to strain your eyes. According to some studies, people who use digital devices regularly blink about half as often in a minute as individuals who don’t use electronics for their jobs. As a result, people who work on a computer are more at risk for developing eyestrain.
In fact, between 50 and 90 percent of people who work with electronics will develop eyestrain at some point in their career.
When you do any of the activities mentioned above, you try to focus on the task as much as possible. That added focus, coupled with minimal blinking, causes you to clench the muscles in your eyelids, temples, face, and jaw so you can use those muscles more. This unconscious clenching of your eye muscles causes you to develop eyestrain.
What Are the Symptoms of Eyestrain?
Most often, you’ll notice a slight discomfort in your eyes if you suffer from eyestrain. However, you should also look out for the following symptoms of this condition:
- Watery or dry eyes
- Double vision
- Blurred vision
- Difficulty focusing
- Increased sensitivity to light
- Pain in your back, neck, and shoulders
- Headaches
- Tired eyes
- Burning or stinging sensations
- Itchy eyes
If you also have a hard time keeping your eyes open, you may suffer from eyestrain. As you work each day, try to notice if you show any of the symptoms listed above. Once you start to show symptoms of eyestrain, you’ll want to make adjustments to treat the condition as soon as possible.
How Do You Treat This Condition?
Because eyestrain is a temporary condition that doesn’t cause eye damage, an optometrist can’t provide medical treatment to help you recover. However, you should schedule an appointment with your eye doctor to get a comprehensive eye exam—especially if you haven’t had an eye exam in the last year and you frequently work on a computer.
In this exam, tell your optometrist about any symptoms you have, as well as how often you use computers, tablets, or other electronic devices. Your eye doctor may then recommend what changes you can make (such as moving further away from your computer) to reduce your pain and discomfort.
Additionally, your eye doctor may recommend that you adjust all forms of lighting you expose yourself to, reduce the amount of glare on your screens, and upgrade your monitors and screens.
Are There Any Ways to Prevent Eyestrain?
Even if you don’t suffer from eyestrain, you can still prevent yourself from developing the condition. Try the following preventative techniques to keep your eyes healthy and comfortable:
- Blink more often.
- Take breaks and look away from your computer screen as often as possible.
- Exercise your eye muscles.
- Adjust your environment so you don’t have to clench your eyes to focus.
- Reposition your screens so they are at the right height and distance away from you.
- Make sure your eyeglasses or contact lens prescription is updated.
- Don’t read text that is too small.
- Use eye drops to keep your dry eyes moist.
Think you suffer from eyestrain? Visit your eye doctor as soon as possible. A certified optometrist can examine your eyes and determine if you have strained your eyes. He or she may also recommend different treatment options and preventative measures than those mentioned above.
To avoid developing eyestrain, use the preventative tips found in the list above as well. For more information about eye health or how an eye doctor can help you maintain good eyesight, read through the rest of our blog.

You can probably think of several celebrities who are constantly wearing sunglasses. Are they only wearing them as part of a public persona, or do they really need them?
Jack Nicholson, for instance. He’s seldom spotted without his signature shades, even when he’s indoors. He even presented the Best Picture Oscar in 2006 while wearing tinted lenses inside some thick, black frames.
Why does Nicholson always wear sunglasses? According to legend, the actor Fred Astaire convinced Nicholson that the practice is the epitome of cool. Nicholson has also said they help him maintain a little more privacy while in public.
What about Bono? The U2 front man also wears sunglasses seemingly all the time. But in 2014, he revealed that he uses the glasses as more than an accessory. He wears them because he’s had glaucoma for over 20 years. The tinted lenses minimize light sensitivity that can occur with glaucoma.
Bono’s example should make it clear that sunglasses do much more than help the wearer look cool—but of course they do that too. Before you pick your next pair of shades, learn how sunglasses protect your eyes and what protective features to look for before you buy.
Why Sunglasses Matter
You may only don sunglasses on the brightest days or during the sunniest hours. But you should wear sunglasses much more regularly. Any time the sun is out, it’s sending down UV rays that can harm your eyes. Several types of these rays can potentially damage your sensitive eye tissues:
- UVA rays. These lower-energy waves can pass through protective atmospheric layers (like the ozone layer) and cloud cover. UVA rays may penetrate your eyes and damage the lens or retina.
- UVB rays. These rays have shorter wavelengths than UVA rays, which makes them more powerful. UVB rays can harm your corneas or your lenses.
- HEV radiation. HEV stands for high-energy visible radiation, which is blue light that we can actually see. HEV radiation has a shorter wavelength than UVA rays, but these rays can still reach the retina and cause damage.
Any combination of these rays can lead to eye tissue damage. A single, large exposure to intense sunlight can damage your eyes, such as if you didn’t wear protective glasses on a sunny skiing trip. However, most sun damage to your eyes accumulates over time, so the tissue damage won’t become apparent until years down the road. This cumulative exposure can lead to eye problems such as:
- Cataracts, the clouding of an eye’s lens that blurs vision
- Macular degeneration, retinal damage that can block out central vision or lead to blindness
- Photokeratitis, a sunburn to the eyes which can cause temporary loss of vision
- Pterygium, a tissue growth on the eye’s surface that can cause astigmatism
Not wearing sunglasses can also make the skin around your eyes more prone to develop skin cancer.
How to Pick Effective Sunglasses
Sunglasses are your best protection against the sun’s harmful rays and the eye conditions listed above. When you shop for a new pair, don’t only look for frames that make a fashion statement. Make sure they have the following qualities as well:
- The lenses should block out 99 to 100 percent of UVA and UVB rays.
- The lenses should filter out 75 to 90 percent of visible light.
- The lenses and the frames together should ideally be larger to protect the area around your eyes more.
Of course, when most people buy sunglasses, they also want to make a fashion statement. You’ll find a wide selection of styles at an eyewear shop. You can find the pair that looks best on your face and matches the current trends—and the glasses specialists at the office can fit your chosen frames with lenses that offer plenty of protection.
If you wear everyday glasses, ask your optometrist about prescription sunglasses. These frames both protect your vision from damaging sunlight and correct your vision so you can see clearly.
Who Needs Sunglasses Most
Really, everyone should wear sunglasses while they are outdoors, but some groups of people have a particularly high need for quality sunglasses:
- Children. Many children spend hours outdoors almost daily, between playing with friends and recess at school. They also have clearer lenses than adults, which means the sun’s rays can penetrate deeper into the eye. If you have kids, buy them sunglasses and encourage them to wear them while they play outside.
- Anyone who works outdoors. Many adults also spend hours outside while they make a living. These individuals include construction workers, coaches and PE teachers, landscapers, mail carriers, and zookeepers. Even people who drive for a living should invest in and wear high-quality sunglasses as much as possible.
- Anyone who takes medications that increase sun sensitivity. Some prescriptions make your body more sensitive to UV radiation. These medications include tetracycline (an antibiotic), sulfa drugs, and many birth control pills. Ask your doctor or optometrist if you aren’t sure whether your prescriptions come with these potential side effects.
Ultimately, no matter who you are, you should have at least one pair of sunglasses, and you should make a habit of putting them on whenever you’re outside. Come to All About Eyes to search for your next pair of sunglasses so you can protect your precious vision.
May is Healthy Vision Month. Check out our tips below to ensure healthy vision and a happier you.








